SilverFit Rephagia - Relearn to swallow
Dysphagia has a very negative influence on the social life of the client
Eating and drinking together is an essential part of social interaction: drinking a cup of coffee, eating out or having a drink. Even mild forms of oropharyngeal dysphagia, such as drooling, can lead to social isolation. Research shows that 36% of people with oropharyngeal dysphagia try to avoid eating with others (Ekberg et al., 2002).
Dysphagia has far-reaching medical consequences
Oropharyngeal dysphagia can lead to dehydration, poor nutritional status, weight loss, respiratory problems, respiratory tract infections or pneumonia (Lim et al., 2009). American research shows that people with serious forms of oropharyngeal dysphagia are three to fifteen times more likely to have serious complications after a CVA (Medicare, 2001-2002).
Despite the impact of dysphagia, a swallowing problem is usually not treated by the speech therapist because the exercises are difficult to explain to the client. Dietary adjustments are often suggested instead. This is a shift of the problem and also has financial consequences. Special diets are expensive because the food has to be purchased and prepared separately and the client following the diet needs special guidance. A study by SilverFit in eight Dutch nursing homes shows that tube feeding costs eight to nine times as much as normal food and that 7 to 22% of clients receive nutritional supplements. For an average nursing home with 70 beds, the food costs tens of thousands of euros extra per year.
What is the SilverFit Rephagia?
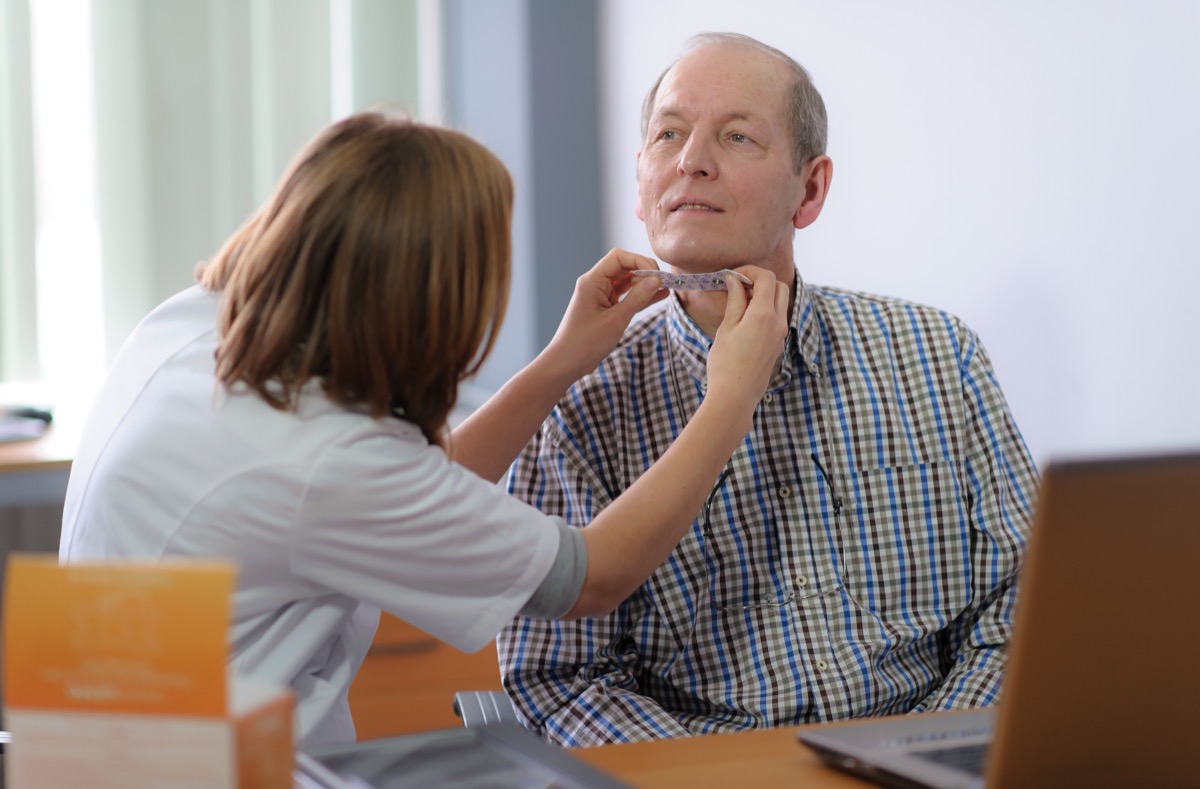
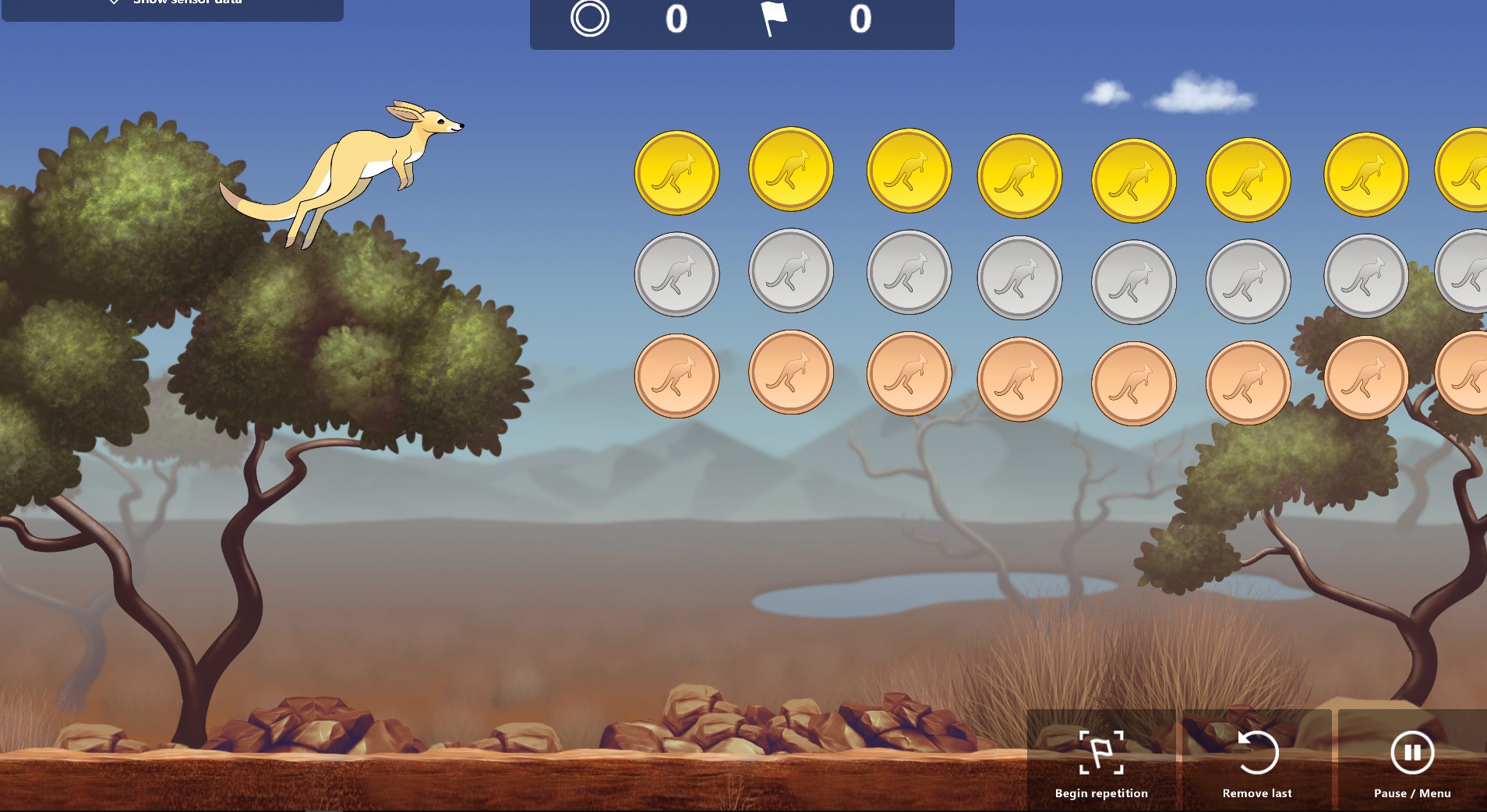
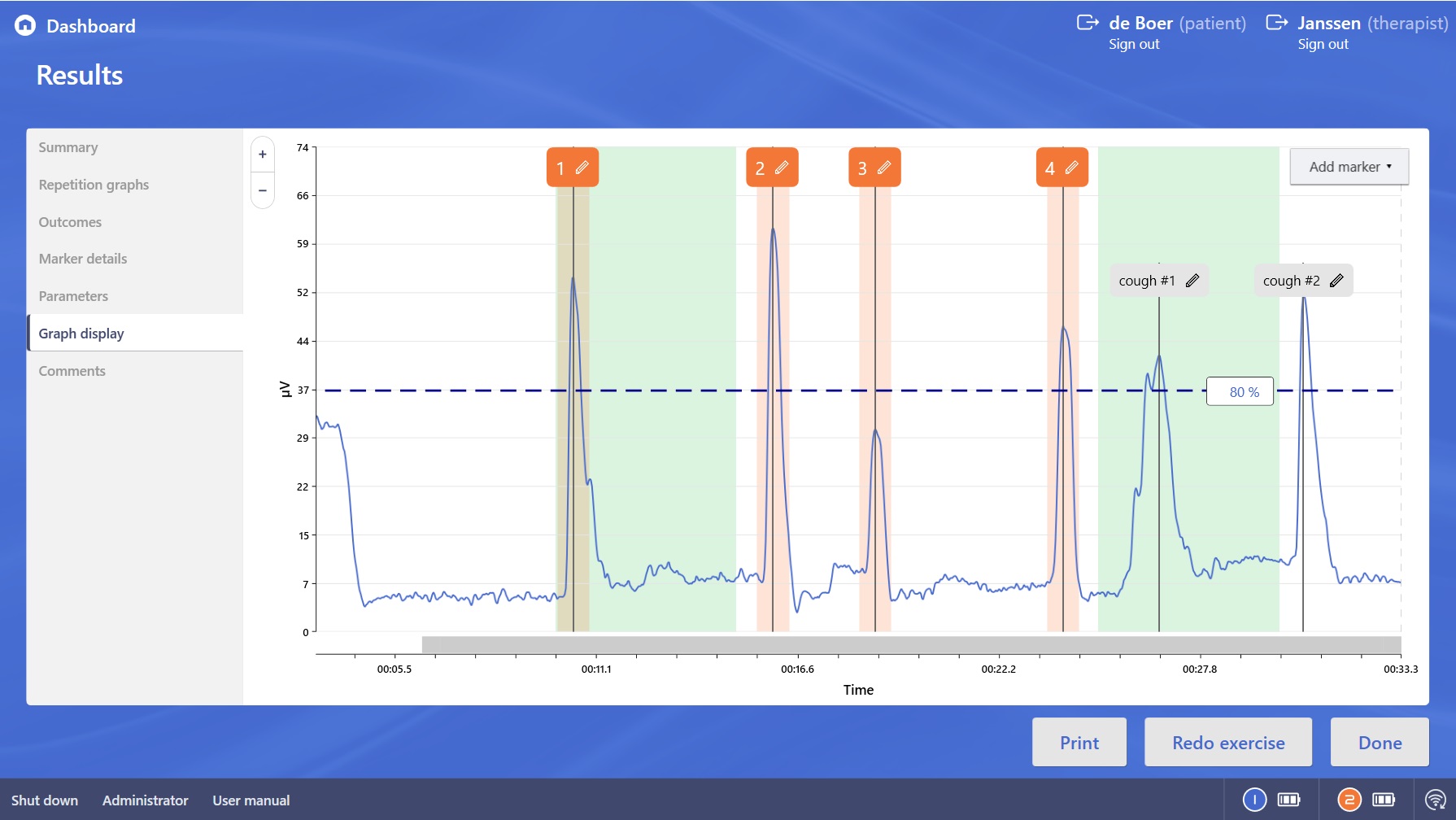
The SilverFit Rephagia is a system that combines existing evidence-based exercises for the treatment of dysphagia with cues and a visual representation of swallowing movement, swallowing power and swallowing timing. The SilverFit Rephagia consists of a laptop with installed software and is supported by the speech therapist. The system can offer any exercise in the form of a computer game or by means of a graph.
Who is the SilverFit Rephagia designed for?
The SilverFit Rephagia has been developed to support adults and the elderly with oropharyngeal dysphagia in their treatment. The system helps to increase the swallowing frequency and swallowing power and to improve coordination (eg through the Mendelsohn Maneuver).
Where is the SilverFit Rephagia used?
The SilverFit Rephagia is used by speech therapists working in (geriatric) residential care centers and rehabilitation centers, the Mental Health Care and hospitals. Speech therapists who work with the SilverFit Rephagia see the number of referrals for clients with dysphagia increasing. A client participates in a series of on average twelve treatments.
The benefits of the SilverFit Rephagia compared to treatment without visual representation
- The exercises are specifically aimed at clients with oropharyngeal dysphagia.
- The speech therapist has a support tool that ensures that the client understands the exercise well and can perform it effectively.
- The speech therapist can use the decision aid to select the correct exercise, method and visualization per client.
- The speech therapist and the client both receive valuable insights into the client's progress.
- The client is motivated to practice thanks to the interactive games.
- The client with reduced cognitive function and / or a mental disability is easier to involve in practicing thanks to the games.
For more information about the SilverFit Rephagia, please contact us.
 Nederlands
Nederlands  English
English  Français
Français  Deutsch
Deutsch